
From the Director
Welcome to Capital Health Cancer Center.
When we decided to rebrand Capital Health’s Oncology Service into a full-fledged Cancer Center, it really served as a catalyst for us to bridge existing clinical gaps we had in our programs. The result is that we now have the capability, in-house, to provide state-of-the-art care across multiple cancer sites.
For example, for the first time in the health system’s more than 100-year history, our staff now includes fellowship-trained colorectal and thoracic surgeons as well as gynecologic oncologists, among other key specialists.

We also now have several Centers of Excellence. These include our Pancreatic Center of Excellence (accredited by the American Pancreas Foundation), the Liver Center of Excellence, the Robotic Center of Excellence (accredited by the Surgical Review Corporation), the Center for Comprehensive Breast Care, the Lung Center of Excellence, the Neuro-Oncology Center of Excellence, and the Retroperitoneal Malignancies Center of Excellence.
The Robotic Center of Excellence is symbolic of our investment in state-of-the-art technologies that lead to improved outcomes in hepato-pancreato-biliary, colorectal, lung, urologic and gynecologic cancers. Because of this investment, and the addition of skilled surgical oncologists well trained in robotic, minimally invasive techniques, Capital Health is among the first centers in New Jersey to perform many of these groundbreaking procedures.
However, our team includes more than just expert surgeons: We also have leading specialists in radiation and medical oncology, interventional radiology, nursing, nutrition, supportive care, and more.
This broad-based expertise allows us to optimize care with a patient-centered approach, one that enables us to focus not only on quality and outcomes but on the satisfaction of those in our care and their families.
The modern facility that houses the Cancer Center opened in 2012 and was designed by an architect based on his own experience at another hospital to include large individual patient rooms that are easy to navigate and state-of-the-art surgical and treatment centers. We also offer free valet parking to all patients and their visitors.
By combining our talent, infrastructure and technology, Capital Health Cancer Center is now able to offer better quality care than large academic medical centers, serving Mercer County and the surrounding counties in New Jersey as well as Bucks County in Pennsylvania.
We hope that you feel confident in referring your patients diagnosed with cancer to us.
Cataldo Doria, MD, PhD, MBA, FACS
Medical Director, Capital Health Cancer Center
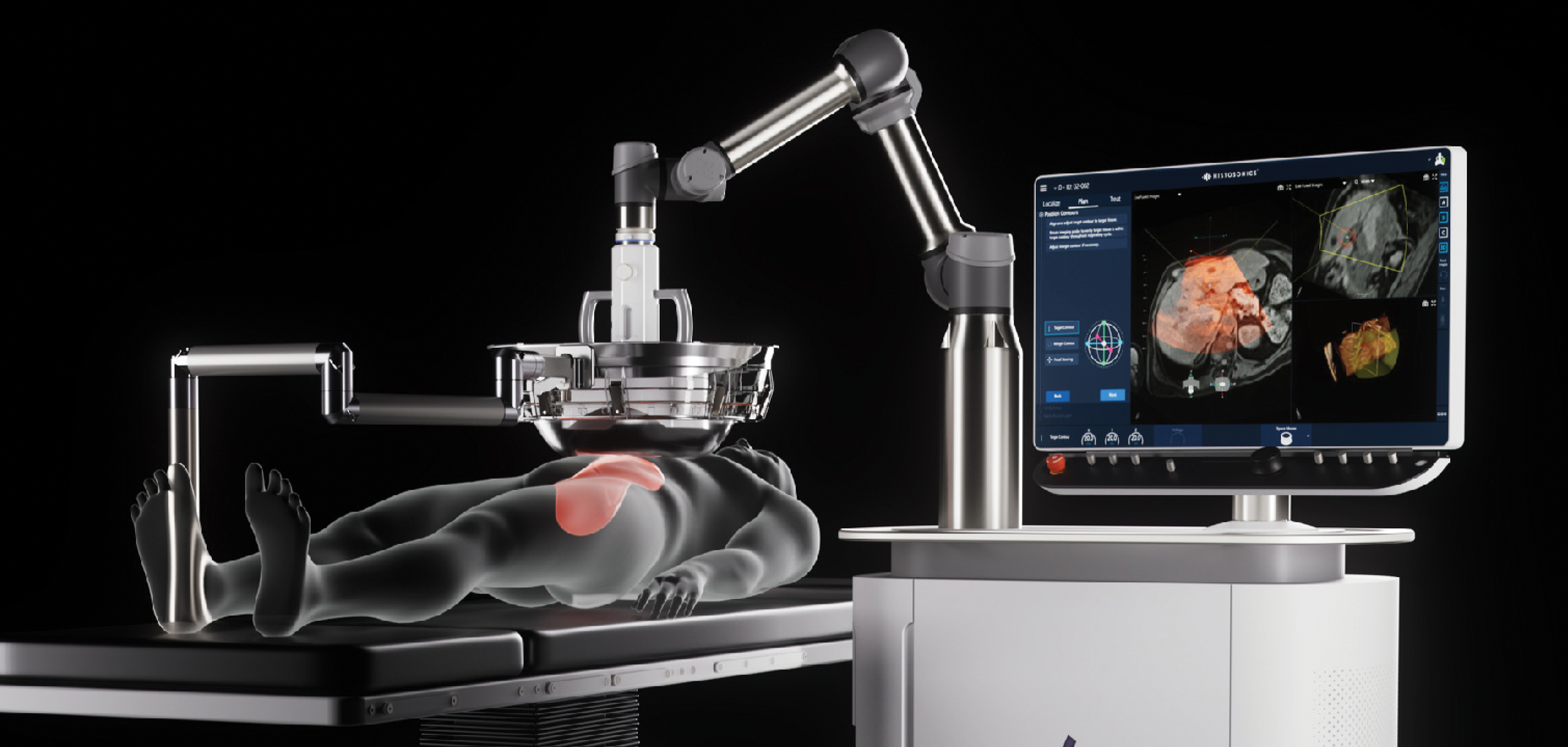
Capital Health to Add Histotripsy Noninvasive Procedure for Liver Cancer
A novel, noninvasive form of focused ultrasound that uses high-amplitude, very short pulses designed to mechanically liquefy and destroy targeted tissue will be coming to Capital Health Cancer Center in the summer of 2025. This technology is currently FDA-approved to treat liver tumors and will soon be approved to treat additional cancer sites.
Histotripsy is a state-of-the-art form of energy-generating device that creates a “bubble cloud,” which in turn, via a phenomenon known as acoustic cavitation, destroys solid masses growing in the liver. The approach was developed by leading ultrasound scientists from the University of Michigan as a noninvasive potential alternative to certain surgical procedures.
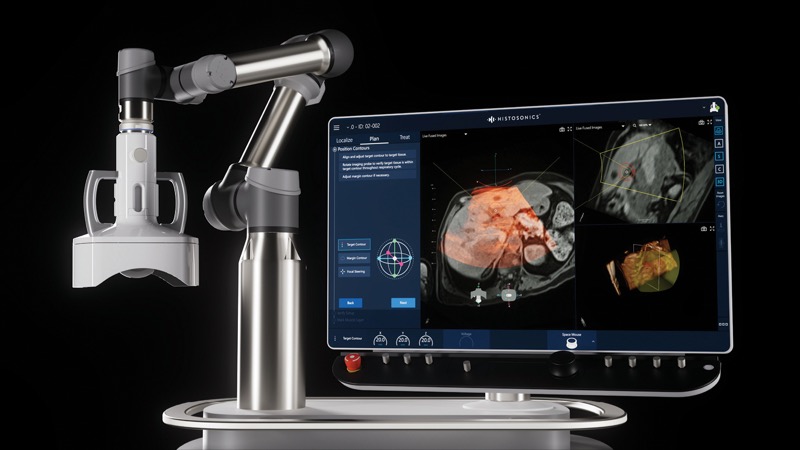
Five-year relative survival rates for liver cancer remain relatively low (at 22%), based on data from the Surveillance, Epidemiology, and End Results (SEER) database maintained by the National Cancer Institute. However, survival rates are higher for people who undergo surgery to remove their cancers, particularly patients with small, resectable tumors who do not have other serious health problems.1
The nonthermal nature of histotripsy enables the technology to overcome many of the limitations associated with thermal devices, such as heat sink effect and lack of precise margins and predictability.2
In research to date, hepatic histotripsy has been shown to effectively destroy cancerous tissue in the liver without any device-related adverse events.3
Once it becomes available next summer, Capital Health Cancer Center will be the only center in the region offering this unique treatment.
- J Cancer. 2019;10(2):494-503.
- Int J Hyperthermia. 2021;38(1):561-575.
- Int J Hyperthermia. 2022;39(1):1115-1123.
Cancer Center Employs State-of-the-Art Diagnostic and Treatment Approaches in Lung Cancer

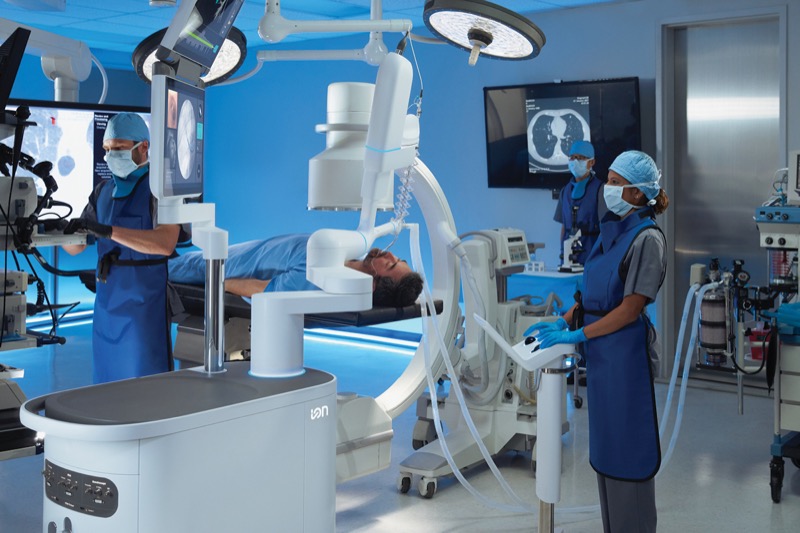
Capital Health Cancer Center offers patients with suspected or diagnosed lung cancer access to the most advanced modalities for the management of the disease in a compassionate and patient-centered environment. This includes the latest noninvasive techniques for lung cancer diagnosis, including endobronchial ultrasound and robotic-assisted bronchoscopy, as well as minimally invasive robotic surgery for patients who will benefit from these procedures.
“We offer patients every possible diagnostic and treatment option for lung cancer right here close to home,” said interventional pulmonologist Diana Kolman, MD, the co-director of the Cancer Center’s lung cancer program with thoracic surgeon James McPherson, MD, MPH.
“Robotic-assisted bronchoscopy allows me to biopsy small nodules in any part of the lung, particularly in the periphery,” added Dr. Kolman, who is board-certified in both interventional pulmonology and critical care. “Not only can I diagnose the cancer, I can also stage the disease at the same time with a biopsy of the lymph nodes in the chest, which allows us to quickly decide whether the patient is a candidate for surgery.”
Smaller lesions, with no lymph node involvement, can typically be treated with surgery alone. Dr. McPherson, who joined Capital Health in the summer of 2024 after a 20-year career in cardiothoracic surgery in California, performs the vast majority of his lung cancer surgeries robotically.
“The advantages of robotic surgery for lung cancer could mean more quickly going back to an active retirement or going back to work, or they could mean proceeding with the next phase of therapy,” Dr. McPherson explained. “For patients with more advanced lung cancer, they will need chemotherapy, immunotherapy and/or radiation, and with a less invasive surgical option, they can start that sooner. The key to beating lung cancer is early diagnosis and treatment.”

Drs. McPherson and Kolman and their team ensure that the time line from patient referral to diagnosis to starting treatment is as speedy as possible. “Typically, we can complete the entire evaluation and have the patient beginning treatment within a month, compared with anywhere from two to three months at many other institutions,” Dr. Kolman said.
Two multidisciplinary tumor boards review each patient’s case and plan of care in light of the latest evidence. For patients whose lung cancer is more advanced and requires additional treatment, Drs. Kolman and McPherson partner closely with other specialists in Capital Health Cancer Center, including Nikhil Thaker, MD, the director of Radiation Oncology. Capital Health is one of the only institutions in the Northeast to offer endobronchial brachytherapy for lung cancer, which involves placing a catheter in the airway at the time of bronchoscopy.
“After I debulk and excise the lesion during the bronchoscopy, Dr. Thaker places the high-dose radioactive seeds directly within the tumor for a short period of time, attacking the cancer from the inside out,” Dr. Kolman explained. “We have had some incredible cases of patients being tumor-free and having a fully reconstructed airway after this procedure.”
For about 20% of patients with lung cancer, the disease invades the pleura (thin layers of tissue covering the lungs and lining the chest cavity) and the pleural cavity, often leading to a buildup of fluid around the lungs. Capital Health Cancer Center now offers an advanced pleural program, in which Dr. Kolman can diagnose and treat the issue in one procedure, while also managing any related airway problems. This means less time in the hospital and quicker relief for patients.
“Many patients with late-stage lung cancer develop obstructions of their airways, causing difficulty breathing,” she said. “With interventional bronchoscopic procedures, I can cut out the tumor, clean up the airway, put in a stent, and give patients an improved quality of life as well as the ability to receive additional treatment.”
Multidisciplinary HPB Team Provides Unique Care Close to Home
Capital Health is taking a multidisciplinary approach to the management of hepato-pancreato-biliary (HPB) cancers, ensuring that patients receive state-of-the-art care before, during, and after treatment—whether it is surgery, chemotherapy, radiation therapy or a combination.
The team-based care strategy incorporates specialists from two separate centers of excellence within the health system: the Liver Center of Excellence and the Pancreatic Center of Excellence, the latter of which is accredited by the American Pancreas Foundation based on surgical volume, outcomes and patient satisfaction, both for those with pancreatic cancer or with chronic pancreatitis.
“There are only a handful of centers so accredited nationally,” said Cataldo Doria, MD, PhD, MBA, FACS, an internationally renowned surgeon who specializes in the treatment of benign conditions and malignancies of the liver, pancreas and bile duct and medical director of Capital Health Cancer Center. “This really speaks to the quality of care we offer.”
Every patient referred to one of the centers for HPB cancers is evaluated during their initial consultation by the multidisciplinary team in a single visit, meeting with surgical oncologists, medical oncologists, radiation oncologists and interventional radiologists and the director of supportive services.

Meeting with this latter provider early in the treatment process allows patients to establish relationships with them and, hopefully, mitigate any emotional stress associated with some of these services, according to Dr. Doria.
“Palliative care is often wrongly associated with end of life, when in reality we rely on some of these approaches throughout treatment,” he explained. “However, if we wait until later in treatment for patients to consult with a supportive care practitioner, patients can become distressed. Our philosophy attempts to avoid this.”
All patients also consult with a nutritionist, both to review possible dietary modifications that may help support treatment and to ensure that they are healthy enough to undergo cancer treatment. Many patients are also assessed by the center’s research coordinator, who may refer them to ongoing clinical trials (depending on eligibility) of novel therapies being conducted within Capital Health.
The patient treatment plan is mapped out prior to their initial consultation during weekly “pre-meetings” attended by the entire multidisciplinary team. As treatment progresses, all cases are discussed in weekly follow-up meetings to ensure that goals are being met and to consider additional therapies, as needed. The patient–provider relationship established before treatment extends well past the initial consultation because the entire team follows patients throughout the process.
“This approach distinguishes us from any other center I’m aware of,” Dr. Doria said. “Many centers require six different visits for what we accomplish in a single visit. After that initial visit, the patient knows the treatment plan. Most patients who require HPB surgery undergo their procedures within two weeks of their initial evaluation.”
Patients who receive chemotherapy, radiation therapy and interventional procedures for their cancer also benefit from the comprehensive approach, according to Ajay Choudhri, MD, director of Interventional Radiology and chairman of Radiology at Capital Health Cancer Center.
Since the addition of Dr. Doria to the team in 2018, Capital Health can now offer HPB cancer patients the minimally invasive robotic Whipple procedure, which allows for the treatment of more advanced disease and brings with it reduced recovery time and postoperative pain, while yielding similar if not better outcomes to traditional, open surgeries. Still, these patients often have pre- and postoperative interventional radiology and imaging needs, Dr. Choudhri said.
He and his team can perform adjunctive procedures such as chemoembolization, intraarterial therapy and stent implantation, as well as drainages and biliary interventions. They also have access to state-of-the-art imaging technology, including PET/CT, 3-Tesla MRI and 256-detector, high-resolution CT.
“We offer the same level of expertise in HPB you would expect at an academic medical center, locally and all under one roof,” Dr. Choudhri noted. “We work hand-in-hand with surgeons, like Dr. Doria, to provide comprehensive care, but with a personal touch.”
Breast Program Boasts Extensive Service Offerings, Welcomes New Physicians

Breast cancer patients treated at Capital Health Cancer Center have access not only to expert treatment but also to a wide range of resources to support them in their cancer journeys. For example, nurse navigators work with each patient to coordinate care and pair them with resources, such as psychosocial, transportation or financial support, and wellness programs are available to nurture patients’ mental and physical health. The breast cancer program also includes plastic surgery services, scalp cooling during treatment, an on-site spa, wig services and a healing garden.
Furthermore, Capital Health Cancer Center has added Yi Huang, MD, a fellowship-trained breast surgeon, to the team who serves as director of Capital Health Center for Comprehensive Breast Care.
“Capital Health has a long track record of having immense talent within the medical staff and a strong commitment to patient care,” said Dr. Huang, who is board-certified in general surgery. “Our comprehensive breast program offers a full spectrum of services to our patients for both benign and malignant breast diseases.”


Also new to the team is Jenna Mancinelli, DO, a fellowship-trained breast surgeon who completed her core general surgery rotation at Capital Health as a third-year medical student.
Both Drs. Huang and Mancinelli are fellowship trained in breast surgery and have dedicated their surgical careers to using the most advanced surgical techniques and latest care options, all with the goal of achieving excellent oncologic outcomes as well as aesthetic results. Their arrival bolsters Capital Health Cancer Center’s long-standing track record of excellence in breast cancer care. In 2025, Capital Health Cancer Center received its third accreditation from the National Accreditation Program for Breast Centers.
“As a multidisciplinary team, we come up with the best approach for each patient’s cancer,” said program co-director Erica Linden, MD. “Breast cancer is a multimodality cancer where treatment is not just surgery or radiation or chemotherapy. It’s all of us working together to tailor the plan to each patient.”
Growing Gynecologic Oncology Program Adds New Expertise, Locations

With the recruitment of a second fellowship-trained gynecologic oncologist in August 2024, Capital Health Cancer Center is expanding its services for patients with all gynecologic cancers—ovarian, uterine/endometrial, cervical, vulvar and vaginal—as well as precancerous conditions of the cervix, vagina, vulva and uterus.
For the past five years, the Gynecologic Oncology Program has been led by Joyce Varughese, MD, an expert in both traditional and minimally invasive surgical approaches to these cancers, including laparoscopic and robotic surgeries using the da Vinci Xi Surgical System (Intuitive Surgical).
When she launched the program at Capital Health Cancer Center in 2019, it was the first gynecologic oncology program in Mercer County, according to Dr. Varughese, who completed her fellowship training in gynecologic oncology and a residency in obstetrics and gynecology at Yale School of Medicine after receiving her medical degree from Albert Einstein College of Medicine in New York City.
Joining Dr. Varughese is Mona Saleh, MD, a native of Hamilton, New Jersey, who received her medical degree and completed her residency in obstetrics and gynecology at New York University Grossman School of Medicine, and a fellowship in gynecologic oncology at Icahn School of Medicine at Mount Sinai, both in New York City.

“I really wanted to come back home and serve the community that raised me,” Dr. Saleh said. “I feel like I understand the people in this area, the challenges they face and the problems they have, and I believe I can contribute positively here. I also speak Spanish and Arabic fluently, so I can communicate with patients from those communities and make a deeper connection.”
With the addition of Dr. Saleh, the practice will be expanding its locations from its primary location at Capital Health Medical Center – Hopewell, to include the Capital Health OB/GYN offices in both Bordentown and Yardley, Pennsylvania.
“This means that new patient visits and surveillance can all happen closer to patients’ homes,” Dr. Varughese noted. “At the Cancer Center in Hopewell, everything is in one building—surgery, chemotherapy and radiation. We also offer extensive patient support services focused on quality-of-life issues both during and after treatment, including nutrition, social work, financial assistance, support groups and palliative care; and we have a dedicated nurse navigator who works closely with patients throughout their care journey.”
“We get new patients in within a week,” Dr. Saleh added. “We are also sensitive to the fact that many of our patients are older women and may have other medical conditions, so we go out of our way to coordinate appointments so that they can see us as well as other specialists on the same day.”
Drs. Varughese and Saleh collaborate closely with the Radiation Oncology Program (see page 11) and with medical oncologists, including Emily Chen, MD, who has practiced at Capital Health since 2007 and received her fellowship training in hematology and oncology at SUNY Downstate Health Services University, in New York City.
“We meet in a multidisciplinary case conference every other week to review all new patients and any new developments with ongoing patients,” Dr. Chen said. “Our patients have access to all the most advanced therapies, including the latest chemotherapy regimens as well as the latest immunotherapies.”
“We have the same surgical offerings as those available in New York City or Philadelphia, as well as the same chemotherapy and immunotherapy medications,” Dr. Varughese added.
Minimally Invasive and Robotic Techniques Distinguish Leading Colorectal Surgery Program

Under the leadership of Ashlee Godshalk Ruggles, MD, the Colorectal Surgery Program at Capital Health Cancer Center has been an early adopter of robotic surgical approaches that improve outcomes.
“Nationwide, approximately 40% of colon and rectal surgery is still done with open incisions, which involve a longer stay in the hospital, more potential complications and more discomfort for the patient,” Dr. Godshalk Ruggles said. “But with laparoscopic and robotic techniques, patients are hospitalized for an average of two days instead of five to seven; they are able to eat much more quickly after surgery; and they experience more rapid return of bowel function.”
For robotic surgeries, she and her team are using the da Vinci Xi (Intuitive) surgical system. In addition to the well-known benefits of robotic surgery (e.g., smaller incisions, less postoperative pain), the system’s advanced camera technology provides finely tuned visualization, and the robotic instrumentation allows for precision stitching.
“We typically use the robot for almost all our cases, which is something you will not find at many other programs,” Dr. Godshalk Ruggles explained. “It allows us to keep all the bowel inside and make much, much smaller incisions.”

In September 2024, Dr. Godshalk Ruggles was joined by John Berry, MD, a double board-certified colorectal and general surgeon with a decade of experience in minimally invasive abdominal and transanal techniques.
“I specialize in complex conditions such as advanced rectal and colon cancer and complex IBD [inflammatory bowel disease],” Dr. Berry said. “These patients are not exactly run of the mill and have more challenging pathologies. For example, we now offer transanal total mesorectal excision and lateral pelvic lymph node dissection for advanced, life-threatening rectal cancer. Transanal total mesorectal excision allows for much greater visualization of the rectal tumor allowing complete resection without a permanent ostomy. Lateral lymph node resection translates to less cancer recurrence in low rectal cancers. When a patient has advanced rectal cancer, you need to be able to offer surgical care that addresses the entire breadth of their disease. These techniques are now unique to Capital Health.”
Capital Health is fully equipped to guide patients through the entire spectrum of rectal cancer care, Dr. Berry said. In fact, the colorectal program is working toward a Center of Excellence designation in colorectal surgery, a distinction that requires programs to meet rigorous, internationally recognized standards in providing the safest, highest-quality care and surgical capabilities.
“We have GYN oncologists, radiation and medical oncologists, plastic surgeons, urologic oncologists, reproductive specialists, geneticists, a first-rate ostomy team, a pelvic health center, tumor site-specific cancer navigators—all of these specialists play a role in your successful rectal cancer care,” Dr. Berry said. “It’s all here.”
Many Cancer Screening Options Offered at Capital Health
At Capital Health Cancer Center, the latest evidence-based recommendations guide screening programs for malignancies, including lung, pancreatic, colorectal, prostate, breast, and cervical cancers. In general, research suggests early diagnosis means more treatment options and better outcomes for patients—hence the importance of screening.
Here is an overview of the approaches Capital Health Cancer Center takes for the following cancers:

- Lung: The U.S. Preventive Services Task Force (USPSTF) recommends annual CT screening for all adults ages 50 to 80 years who have a 20-cigarette pack-year smoking history (e.g., two packs a day for 10 years or one pack a day for 20 years) and currently smoke or have quit within the past 15 years, according to director of Thoracic Surgery and co-director of the Lung Center of Excellence James McPherson, MD, MPH.
- Pancreatic: Those at high risk are offered CT, MRI and magnetic resonance cholangiopancreatography scans; genetic testing; and endoscopic ultrasound (EUS), the highest-resolution imaging test available for the pancreas. Those with BRCA1 and BRCA2 mutations and/or hereditary pancreatitis and new-onset type 1 diabetes after age 50, for example, generally have a 3% or higher lifetime risk for pancreatic cancer, noted Jason Rogart, MD, the director of Interventional Gastroenterology and Therapeutic Endoscopy at Capital Health Center for Digestive Health. “For most high-risk individuals, we will do one imaging study a year, typically alternating between EUS and MRI,” he said. “We’re one of the only centers in the area performing a high volume of EUS procedures.”
- Colon: All low-risk adults should receive screening colonoscopies beginning at age 45, and every 10 years thereafter; those with a family history of colon cancer or advanced polyps should begin at age 40, or 10 years younger than the age at which the immediate family member was diagnosed, whichever is earlier. The Cancer Center’s direct-access colonoscopy program makes it easy for patients to schedule an appointment, using an online form (see box), according to Ashlee Godshalk Ruggles, MD, medical director of Colorectal Surgery.
- Breast: Annual screening mammograms for breast cancer should begin at age 40 years for most low-risk individuals. Patients with a positive family history should begin screening 10 years before the youngest first-degree relative was diagnosed; for those with a genetic mutation, annual screening should begin with MRI at age 25 years. Capital Health offers state-of-the-art 3D mammography at all its locations, and appointments usually can be scheduled within two to three weeks, also using an online form (see box). For high-risk patients, the Cancer Center offers supplemental testing, such as breast MRI and whole-breast ultrasound, said Erica Linden, MD, director of Breast Oncology and Cancer Genetics.
- Cervical: Screening, via Pap smear, is recommended for all females beginning at age 21 years, with cervical cytology alone every three years between ages 21 and 29 years. From ages 30 to 65 years, the recommendations are for cervical cytology alone every three years, HPV (human papillomavirus) testing alone every five years, or co-testing every five years. After age 65 years, if adequate prior screening has been completed, no further testing is recommended. “Our robust obstetrics and gynecology department has more than half a dozen locations in Mercer County and Bucks County where patients can be seen for cervical cancer screening,” said Joyce Varughese, MD, medical director of Gynecologic Oncology.
- Prostate: Given the risk for overdiagnosis associated with prostate-specific antigen (PSA) testing levels, recommendations for screening initiation and intervals differ between leading organizations such as the USPSTF, the American Urologic Association, the National Comprehensive Cancer Network, and the American Cancer Society. Capital Health Cancer Center experts believe PSA testing should be considered for all men beginning at age 50 years in consultation with their primary care physician. For low-risk individuals, the recommended intervals between PSA testing vary between every two to four years, according to Eric Mayer, MD, director of Urologic Robotic Surgery. For men of African American ancestry or those with a first-degree relative who had prostate cancer before age 65 years, screening should start at age 45 years. “We have noninvasive modalities to screen people further, including multiparametric prostate MRI, which allows us to localize areas of concern for targeted biopsies, thereby enhancing detection, and has reduced the overall number of patients requiring biopsy procedures by nearly 50%,” Dr. Mayer said.
Scheduling a Cancer Screening with Capital Health

Integrated Neuro-Oncology Team Provides Expert Multidisciplinary Care

The Neuro-Oncology Program at Capital Health Cancer Center leverages expertise from multiple specialties to provide optimal care for patients with brain cancer.
“The thing that sets our program apart from other centers, not just in the local area but in the entire region, is the specialized expertise of the people involved in the care and treatment of patients who battle brain and/or spine cancer,” said Michael Salacz, MD, director of Medical Neuro-Oncology at Capital Health Cancer Center. “Because all brain cancers are rare, there are very few true specialists in practice. So, it’s unusual to have this degree of expertise and experience at one center.”
Patients are in skilled, caring hands in the Neuro-Oncology Program. Dr. Salacz and colleagues Navid Redjal, MD, director of Neurosurgical Oncology, and Nikhil Thaker, MD, medical director of Radiation Oncology, bring many years of specialized experience and a patient-centric approach to the team.
“Dr. Redjal is a Harvard-trained neurosurgeon who has been in practice for over a decade now, and his area of specialty is brain tumor surgery. His expertise extends to complex brain surgery such as awake brain tumor surgery, which integrates functional imaging to safely maximize tumor removal without affecting critical brain function. Dr. Thaker’s primary interest is in central nervous system tumors. He is an MD Anderson–trained radiation oncologist with nearly 10 years of experience. In terms of the connections, the skill set and the knowledge base here, it’s just enormous,” Dr. Salacz said. “I trained at Duke, and I’ve been doing this now almost 20 years. I approach patient care and treatment from both a neuro-oncology—specific and a palliative medicine mindset, seeking to balance treatment effectiveness with side effects.”
A diagnosis of brain cancer can be daunting, but patients treated in the Neuro-Oncology Program at the Cancer Center have access to this team of physicians with deep, specialized expertise who collaborate seamlessly to tailor their treatment approaches.
“We aim to provide the most cutting-edge care with the highest level of compassion to get the patients through the process,” Dr. Redjal said.
“Our goal is always to minimize any collateral damage to normal brain tissue and maximize treatment of cancer by using high-tech tools with minimally invasive approaches,” he added.
Treatment for brain cancer does not necessarily require invasive procedures. At the Cancer Center, the Neuro-Oncology Program offers noninvasive approaches including CyberKnife (Accuray) radiosurgery, which uses a robotic system to administer precise, high-dose radiation to target and treat malignant tissue in the brain while minimizing damage to surrounding tissues and maximizing quality of life. Patients are able to go home the same day of treatment.
“We have a dedicated medical neuro-oncologist who has expertise in treating patients with the most advanced systemic treatments based on molecular pathology,” Dr. Redjal said. “Some of the newer treatments with targeted therapy are available here at Capital Health.”
Drs. Redjal and Salacz emphasized the importance of having a supportive team as part of cancer care. A neuro-oncology navigator connects with patients as they enter treatment to help guide them through their cancer journey, coordinating with clinicians to facilitate a smooth treatment process. The close-knit neuro-oncology team also holds a weekly multidisciplinary clinic, which enables patients and families to meet with multiple specialists during a single visit. It also fosters the development of a multidisciplinary treatment plan for all patients.
“It’s already painful enough to get a cancer diagnosis. We try to lessen the pain for patients by eliminating the need for multiple appointments with different physicians,” Dr. Redjal said. “In this way, we minimize the patient’s inconvenience, eliminating the need for traveling to different providers. In a single multidisciplinary visit, we provide a consistent comprehensive plan talked through with all the different providers centered on the patient.”
Advanced Diagnostics and State-of-the-Art Therapies in Urologic Oncology
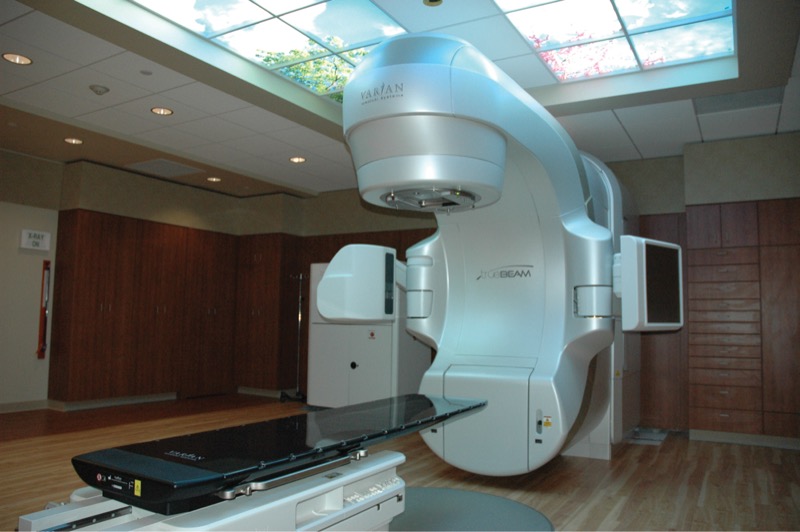
With some of the most sophisticated technology and surgical techniques currently available in the field, the Center for Urologic Oncology at Capital Health Cancer Center offers patients with prostate, testicular, kidney and bladder cancers access to leading-edge care with the best possible outcomes. Led by renowned urologic surgeon Eric Mayer, MD, director of Urologic Robotic Surgery and director of the Center for Urologic and Retroperitoneal Malignancies, the program offers advanced diagnostics and state-of-the-art therapies, such as minimally invasive robotic surgery with the da Vinci Surgical System (Intuitive Surgical), CyberKnife (Accuray) and TrueBeam (Varian) external beam radiation therapy. Patients benefit from a tailored approach designed to combat their specific cancer type and stage.
“We recently operated on a patient with testicular cancer that had metastasized to the abdomen and involved multiple organs, including the kidney and colon,” said Dr. Mayer, the first surgeon in Pennsylvania to perform a robotic-assisted laparoscopic prostatectomy using the da Vinci Surgical System. “Working with our medical oncology colleagues, we first treated him with chemotherapy to downsize the tumor, and then were able to surgically remove the residual tumor along with the left kidney and a portion of the colon and aorta, and render him disease-free. Surgeries such as these are typically only performed at a handful of academic centers, but now patients in central New Jersey and Bucks County can receive this kind of advanced care close to home.”
The majority of cases managed by the Urologic Oncology Program involve laparoscopic, minimally invasive interventions, such as robotic partial nephrectomies to preserve kidney function in localized kidney cancers, robotic cystectomies for bladder cancer, and robotic prostatectomies.
The surgical team works closely with radiation oncologist Nikhil Thaker, MD, medical director, Radiation Oncology, who completed his residency at The University of Texas M.D. Anderson Cancer Center and is double board-certified in radiation oncology and clinical informatics.
“Our Urologic Oncology Program is extremely multidisciplinary, with radiation oncologists and pathologists coordinating with surgeons and meeting every one to two weeks for multispecialty consultations and evaluations,” Dr. Thaker said.
Patients usually receive their initial consultations at the newly renovated facilities in Hopewell or at Capital Health’s multispecialty offices in Newtown, Pennsylvania. “We have an oncology nurse navigator specifically dedicated to urology, and she is able to obtain imaging and other records that are needed so that the patient can be seen quickly,” Dr. Mayer said.
The Center for Urologic Oncology also recently received a grant from the National Institutes of Health, in partnership with Pennsylvania’s Baruch Blumberg Institute, to develop a novel urinary screening test to detect bladder cancer. The goal is to develop a simple urinary test that could replace upper-tract imaging and endoscopic procedures for initial bladder cancer detection.
“In addition to the potential for a more precise method of detection, a urine test for bladder cancer would put much less of a burden on patients in the future who are grappling with the uncertainty of a possible cancer diagnosis,” Dr. Mayer said.
Leading-Edge Technology Distinguishes Radiation Oncology Program
The Radiation Oncology Program at Capital Health Cancer Center is incorporating state-of-the-art treatment and diagnostic technologies to optimize outcomes across a variety of cancers.
Patients with prostate cancer referred to the Cancer Center now have multiple options, including the TrueBeam (Varian) radiotherapy and CyberKnife (Accuray) stereotactic radiosurgery as well as high dose-rate (HDR) brachytherapy. The radiation oncology team plans to add the Edge (Varian) stereotactic radiosurgery platform to its toolbox within the next year or so, according to Nikhil Thaker, MD, medical director of Radiation Oncology at Capital Health Cancer Center.
“With the Edge, if a tumor has shrunk, grown or otherwise changed, or one of the normal organs is very close to the radiation field, we can create a completely new radiation plan almost immediately, while the patient is on the radiation table,” he said. “Edge allows us to take extremely high-resolution, diagnostic-quality scans of patients on the treatment table every day before starting highly focused and precise radiation therapy. We can also make very minor, sub-millimeter corrections for a patient’s body position in real time.”
Within the next two years, the Cancer Center will also be on-boarding the Ethos (Varian) radiotherapy platform, which uses artificial intelligence (AI) technology to adapt to daily changes in the shape and position of tumors to deliver the optimal dose to the most effective treatment target. This technology can be used on a variety of tumor sites and types. In addition to the aforementioned technologies, the Radiation Oncology team is using image-guided radiation therapy and HDR brachytherapy, which involves placing high-energy radioactive sources directly within or next to the tumor for a short period of time. The robust and growing HDR program treats multiple malignancies, including cervical, endometrial, skin and lung cancers, and many others.
“We are one of the only institutions in the Northeast to offer endobronchial brachytherapy, which involves placing an HDR brachytherapy catheter in the airway at the time of bronchoscopy for lung cancer, working in partnership with interventional pulmonologists,” Dr. Thaker explained. “This treats disease inside the airway and reduces the risk of obstruction and bleeding.”
The Cancer Center has also added state-of-the-art imaging platforms such as a multi-slice scanner for CT, 4D CT and breath-hold simulations, and advanced 3T MRI.
“Dr. Thaker has a great vision for how he wants radiation oncology at Capital Health Cancer Center to grow, and I am very excited to be a part of this team,” added radiation oncologist Manuj Agarwal, MD.
“We’re committed to treating the whole person, not just the disease,” he added. “Our goal is to provide a supportive and comfortable environment that addresses the social, emotional and physical aspects of each patient’s journey.”
Capital Health Surgeons Leading the Way in Robotic, Minimally Invasive Approaches for Multiple Cancers
Surgical oncologists at Capital Health Cancer Center have been early adopters of robotic technologies that have enabled the use of minimally invasive approaches in most procedures across many tumor sites, including the pancreas, bile duct and liver; colon and rectum; uterus; prostate; and lung.
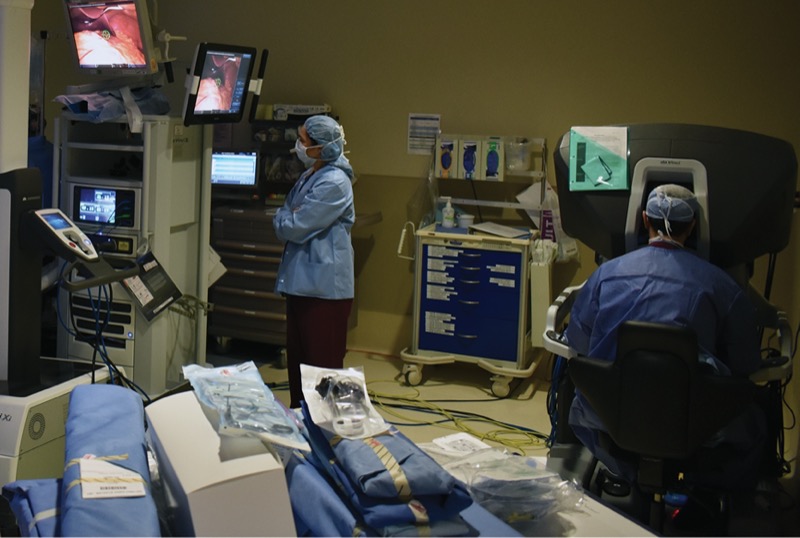
Designated a Center of Excellence in Robotic Surgery by the Surgical Review Corporation, the Cancer Center has expanded its arsenal of da Vinci Xi (Intuitive Surgical) surgical systems to three and added a second console, which means two surgeons can work together using the device for complex procedures. The platform features four robotic arms and 3DHD vision, Firefly fluorescence imaging, integrated table motion and versatile instrumentation—all designed to enhance surgical precision and efficiency.
Capital Health Cancer Center also has a da Vinci SimNow surgical simulator to train surgeons in the use of the technology. The addition of more beds in the operating room that integrate with the da Vinci Xi has further expanded surgical capacity.
Altogether, the Cancer Center’s three da Vinci Xi systems are now used in more than 3,000 procedures annually. In many cases, thanks in part to the smaller incisions used in robotic procedures, cancer patients who undergo surgery with the device have shorter hospital stays, faster recovery times and less postoperative pain, according to Cataldo Doria, MD, PhD, MBA, FACS, medical director of Capital Health Cancer Center and a world-renowned hepato-pancreato-biliary (HPB) surgeon. In some cases, the robot allows surgeons to use new techniques for tumors once considered untreatable.
“As we have expanded the oncology services from a collection of independent offices into a full-fledged, standalone cancer center, we have added to our team of surgical oncologists to include those who specialize in robotic techniques because we believe in the technology and its benefits,” Dr. Doria said. “As a result, we have converted many of our procedures from open to completely robotic.”
In Dr. Doria’s own specialty, HPB cancers, Capital Health was one of the first centers in New Jersey to perform very complex pancreatic cancer surgeries robotically, including the Whipple procedure. The procedure itself has been used for more than a century via open surgery, but has more recently evolved into a minimally invasive technique with robotics.

“Like any other minimally invasive surgery, it offers a number of advantages,” Dr. Doria said. “Some research has also suggested that the risk for infection is lower with the robotic procedure.”
Capital Health’s comprehensive colorectal surgery program, led by Ashlee Godshalk Ruggles, MD, has also strived to expand access to minimally invasive surgical techniques for cancers of the colon and rectum. Now, 95% of her cancer surgeries are performed robotically, well above the national percentage. With robotic surgery, patients recover bowel function much faster, which means they can return to a normal diet much sooner following surgery and have a lower risk for postoperative hernia.
In addition, the use of minimally invasive approaches has become the standard of care for uterine cancer staging, as research has shown there is no difference in patient survival between laparoscopic and open procedures in this setting, according to Joyce Varughese, MD, medical director of Gynecologic Oncology at Capital Health.
“The da Vinci Xi system enables us to perform sentinel lymph node biopsy laparoscopically, and most of these patients go home the same day as their surgery,” she said.
More extensive lymph node dissection also aids in staging lung cancer patients robotically, according to thoracic surgeon James McPherson, MD.
Meanwhile, under the leadership of Eric Mayer, MD, director of Urologic Oncology at Capital Health, surgeons are using the da Vinci Xi system for the vast majority of prostate, kidney, adrenal and bladder cancer cases, with some very large tumors in the kidney being among the few exceptions. For kidney cancer, the technology allows Dr. Mayer and his colleagues to effectively perform partial nephrectomy to excise the tumor and reconstruct the organ, which “maintains function and ensures strong oncologic outcomes,” he said.
“With the da Vinci Xi system, visualization is improved compared with the naked eye; so, with the kidney, where cancerous lesions can be tucked away, it’s a huge advantage in ensuring you get adequate margins,” said Dr. Mayer, who was the first surgeon in Pennsylvania to perform a robotic prostatectomy using the da Vinci Xi system in 2021.
“In addition, the articulation of the smaller instruments on the platform allows us to do maneuvers we can’t do by hand when we’re working on the prostate, which is often difficult to see,” he added. “This gives us more possibilities than we had with open procedures in terms of being able to both access tumors and remove them.”
Even with the movement toward robotics, Cancer Center surgeons are also well versed in traditional, open procedures for patients not suited for surgery using the da Vinci Xi system, Dr. Doria noted.
“Our surgical practice is now extremely competitive in the region and nationally because of our use of robotics, and part of that has been fueled by our recruitment of surgeons with vast experience using the technology,” he said.
Medical Oncology Team Advances Care Through Expertise and Innovation
The Medical Oncology Program at Capital Health Cancer Center provides state-of-the-art, comprehensive, patient-centered, personalized care based on a multidisciplinary team that leverages the skill sets of individual specialists in the delivery of innovative treatments, such as precision medicine approaches.
“We have a team of well-trained and experienced medical oncologists, nurse practitioners, nurse navigators and nurses. We have a robust, busy outpatient and inpatient practice,” said Pamela Crilley, DO, a medical oncologist at Capital Health Cancer Center. “The medical oncologists care for patients with solid tumors, hematologic malignancies and benign hematologic conditions.”
“We organize patients’ treatments working closely with the infusion rooms and radiation oncology, interventional pulmonology, interventional radiology, GI subspecialties and multiple surgical specialties,” added Kristina Zarkua, MD, another medical oncologist at the Cancer Center. “We have dedicated groups in the Cancer Center, such as the lung cancer multidisciplinary group, the GI cancer group, the neuro/central nervous system group, the breast cancer group, the genitourinary group, and hematologic malignancies.”
This subspecialization is supported by strong collaboration across disciplines. “Cancer care is very complicated, so you want to be able to have that real-time, quick turnaround in coordination of care,” said Hongyan Liang, MD, medical director of Digestive Medical Oncology at Capital Health Cancer Center, adding that the program’s integrated approach ensures patients receive the most effective and timely care. “We get patients in and moving on their treatment quickly in a very coordinated way. I really think it’s the best way to get your cancer care.”
Patients treated by the Cancer Center’s medical oncologists have access to cutting-edge cancer treatment approaches, such as precision medicine and immunotherapy, which are transforming the oncology field. The Cancer Center is a National Cancer Institute Community Oncology Research Program (NCORP) affiliate site, meaning patients have access to clinical trials and treatment delivery studies available only at top institutions worldwide. As an NCORP site, the Cancer Center’s team of experts help patients gain access to clinical trials across a broad range of care benchmarks, including symptom management, prevention, screening, and quality of life.
“The idea of chemotherapy for everyone is going away. Precision medicine and immunotherapy help us save our patients from many of the toxicities that come with traditional chemotherapy,” Dr. Zarkua noted. “Guidelines change extremely fast; every year, we have a new set of guidelines. Many new treatments are being approved, and cancer has become a chronic disease. Patients live longer, even with advanced metastatic disease, and they can maintain their quality of life.”
Capital Health’s Research Program Provides Access to the Latest Cancer Treatments
Patients treated at Capital Health Cancer Center can enroll in clinical trials and research initiatives that provide access to the latest cancer treatments. The Cancer Center’s research program is a multidisciplinary collaboration among dedicated specialists who identify and connect eligible patients to these opportunities.
“Each research coordinator participates in tumor boards and is assigned a specific tumor site,” explained Neena Shetty, manager of research for the Cancer Center. “At the tumor boards, they screen for patients, and also regularly interact with the doctors to see if there are any patients that may be eligible for the trials that are open here.”
After identifying a patient for a research study, the coordinators collaborate with the patient and their doctors to discuss the study details. If the patient is interested in participating, they proceed with obtaining consent and enrolling the patient in the study.
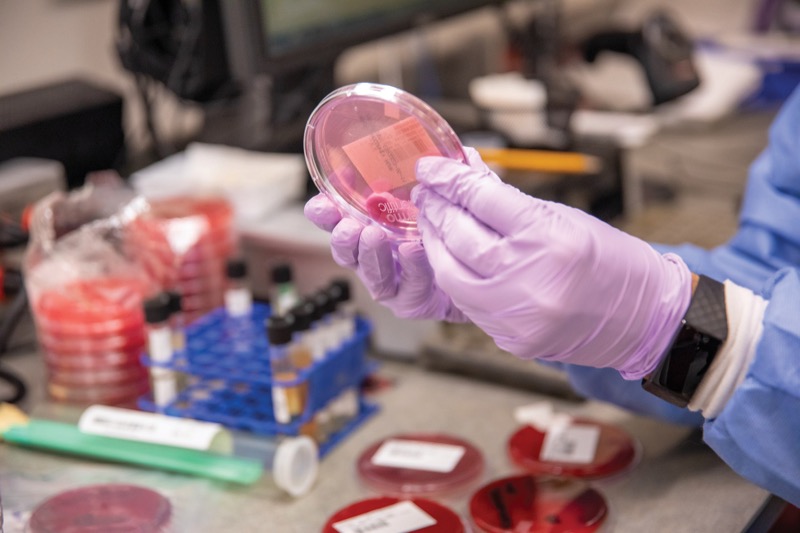
Among the available programs is the biorepository, a large bank of tissue samples collected from patients who are interested in contributing to research. Data collected from the biorepository have shed light on novel biomarkers in liver cancer, and work is ongoing to identify biomarkers in pancreatic cancer. Biorepository data also laid the foundation for work that led to the Cancer Center’s recent grant from the National Institutes of Health (NIH) for work in urology. The NIH grant is the result of collaboration between the Cancer Center and the Baruch S. Blumberg Institute, in Doylestown, Pennsylvania. Capital Health has created a postdoctoral position to further facilitate synergy between scientists and clinicians with the health system and the Blumberg Institute.
The NIH grant is the first of its kind at Capital Health and supports work by Eric Mayer, MD, director of Urologic Oncology, and his team to develop a screening tool to detect bladder cancer from urine samples. The trial is enrolling patients with established bladder cancers to test the assay.
“The preliminary results have been excellent,” Dr. Mayer said. “If it comes to fruition, it’s a very simple test and, thus far, at least in our early work, has been upwards of 90% sensitive and specific. There’s nothing in the commercial space right now that comes close to that.”
Many more exciting trials are ongoing at the Cancer Center. Navid Redjal, MD, FAANS, director of Neurosurgical Oncology, and his team are exploring an approach with TVAX Biomedical Inc. to treat patients with glioblastoma multiforme, the most common and aggressive primary brain cancer. The TVAX protocol harnesses a patient’s immune system to fight this cancer. The trial is currently enrolling participants.
Many more research programs are available for patients to take advantage of and can be found on the Research Program’s website.
“Being able to offer this closer to home is something that’s really helpful to our patient population,” Dr. Shetty said.
Cancer Genetics Program Provides Counseling, Resources for Oncology Patients and Their Families

For many patients, a cancer diagnosis comes with genetic risks that may impact other family members and affect health care decision-making. For more than 20 years, Capital Health Cancer Center’s Genetics Program has provided resources and support for people with cancer and their families. The program is led by medical director Erica Linden, MD, and includes genetic counselor Erin Shehan, nurse coordinator and Cancer Center Director Rona Remstein, and assistant genetic counseling navigator Nina Earle.
“The program offers genetic counseling and genetic testing services to patients who may have a history of cancer themselves and were either diagnosed at Capital Health Cancer Center or elsewhere in the community,” Remstein explained. “We also see patients with colon polyps, patients with a family history of cancer, or patients with a positive genetic test result or mutation for patients who have been tested elsewhere and need an explanation about what their genetic test means. The Cancer Genetics Program will help interpret it for them.”
The Cancer Genetics Program provides counseling and testing services for all cancer types. Patients enter the program from several avenues. Many are referred by their oncologists, but primary care physicians, gynecologists and endocrinologists can also refer patients who may benefit from the program’s service offerings. Patients can also refer themselves through the Cancer Genetics Program website.
During the initial intake process, patients meet with the genetic counselor and genetic counseling navigator to assess the risk factors and genetic predisposition for cancer. The team reviews the patient’s family history going back at least three generations.

“There are models to estimate how likely it is that someone harbors a genetic mutation for a breast, ovarian, or colon cancer syndrome, or some other unique genetic syndrome. These results may impact how frequently patients are screened, at what age they start screening, if they do supplemental screening, or if there are other methods of prevention, including surgery or medication,” Dr. Linden said.
If a patient then wants to undergo genetic testing, the team will work with the patient’s insurance to identify appropriate testing and collect blood or saliva samples to be sent to a genetics laboratory for evaluation.
“We do state-of-the-art genetic testing, not just for one gene or isolated genes, but even panel testing that can include eight, 20 or even up to 80 genes in the appropriate setting,” Dr. Linden noted.
The team will share the testing results with the patients and provide support and resources as necessary. For patients with positive results, the team will review recommendations, put together a plan for the patient and counsel them on subsequent testing for themselves and other family members. The team compiles all testing information into a summary letter for the patient and will share the results with whomever the patient requests.
“We’ve always believed in comprehensive genetic counseling. There’s a lot that’s involved with this because a positive test can affect an individual, but it also affects the family,” Remstein said. “We help these individuals cope with these results, and help them problem-solve.”

Copyright © 2025 All rights reserved. Capital Health Cancer Center unless otherwise noted.
Reproduction in whole or in part without permission is prohibited.

